PrEP’s promise to change the course of HIV has succeeded — but only for white gay men
A decade into the era of the HIV prevention pill, called PrEP, efforts to leverage its heralded power to curb new infections have stagnated in the United States.
This shortfall is a key reason the nation lags far behind many others in combating HIV, with a national epidemic long plagued by racial inequities and only a modestly declining new infection rate.
“We are reaching a scientific crisis in HIV prevention,” LaRon Nelson, an associate professor of nursing and public health at Yale University, said last month at the Conference on Retroviruses and Opportunistic Infections in Seattle. Nelson lamented the gulf between PrEP’s impressive performance in major studies and its moderate real-world impact.
On the bright side, PrEP, which is short for pre-exposure prophylaxis and involves taking either oral or injectable prescription antiretroviral medications in advance of potential HIV exposure, has indeed achieved substantial popularity — but only among white gay and bisexual men, who have long seen a dropping HIV rate.
Such inequity persists despite the efforts of a nationwide public-health army and countless millions of dollars spent promoting and facilitating PrEP use among Black and Latino gay and bi men. Of all major intersectional demographics, these groups contract HIV at the highest rates, and transmissions among them have flatlined or barely declined in recent years.
And so, even amid the national reckoning over racial inequity, PrEP has only served to widen HIV-transmission racial disparities among men who have sex with men.
According to the Centers for Disease Control and Prevention, gay and bi men account for 70% of new cases of the virus. Whites in this demographic comprised 15% of the 34,800 HIV transmissions in 2019, while the much smaller populations of their Black and Latino peers comprised a respective 26% and 23% of new cases.
Additionally, more than a year after the approval of a long-acting injectable form of PrEP, ViiV Healthcare’s Apretude, few are receiving it. Insurers have mostly refused to cover the expensive drug. Consequently, even after clinical trials found injectable PrEPwas dramatically superior to oral PrEP at preventing HIV on a public health level, especially among Black gay men, Apretude’s potential will likely remain untapped for the foreseeable future.
Troubling statistics
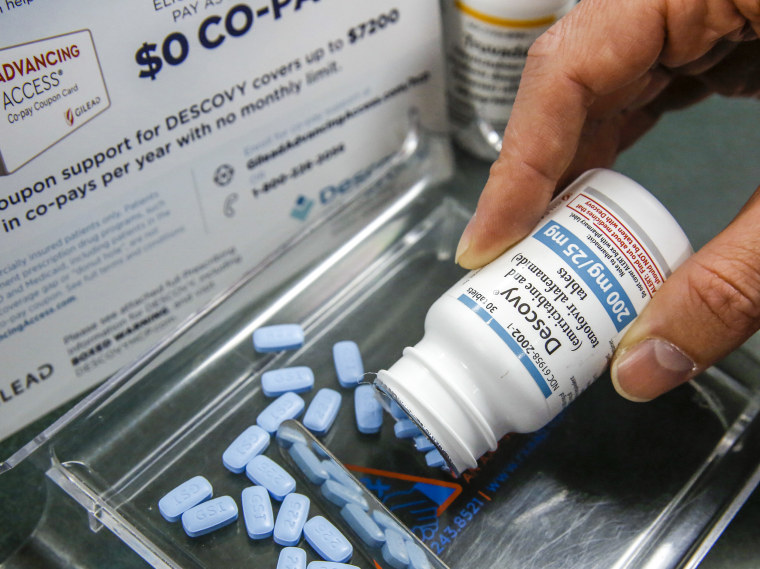
Gilead Sciences’ two-drug combo pill Truvada was approved as PrEP in 2012 and was followed in 2019 by a similar drug, Descovy. When either drug is taken daily, this lowers the risk of HIV by at least 99% among gay and bi men and transgender women, according to multiple studies.
PrEP has helped drive down HIV rates in cities where it has achieved a critical mass of popularity, such as in New York, San Francisco andSeattle. But nationally, PrEP has failed to move the needle by much.
The CDC estimates annual HIV transmissions declined by only 8%between 2015 and 2019. Cases are even rising in some states where HIV prevention investment is lacking, such as Tennessee, where Republican Gov. Bill Lee recently compounded the factors worsening his state’s epidemic by blocking $8.3 million in annual CDC prevention funding.
Approximately 814,000 gay and bi men in the U.S. are good PrEP candidates, the CDC estimates. Between 2017 and 2022, the number of people using PrEP, who have always overwhelmingly been gay and bi men, at any point during each given year increased from 155,000 to 382,000. However, a CDC study presented in Seattle found that in September 2022, just 187,000 people were on PrEP within that 30-day window, suggesting that many people do not take it for long.
PrEP’s increasing popularity likely could have put a major dent in the national HIV rate had its use more closely reflected viral-transmission demographics, according to HIV prevention experts. Of the CDC’s estimate of 21,900 new HIV cases in 2019 (the most recent year for which the agency has produced a transmission estimate) in the three largest racial groups among gay and bi men, a respective 23%, 41% and 36% were in whites, Blacks and Latinos. But a lopsided 69% percent of PrEP users last year were white, while only a respective 9% and 18% were Black and Latino.
Apretude’s approval promised progress
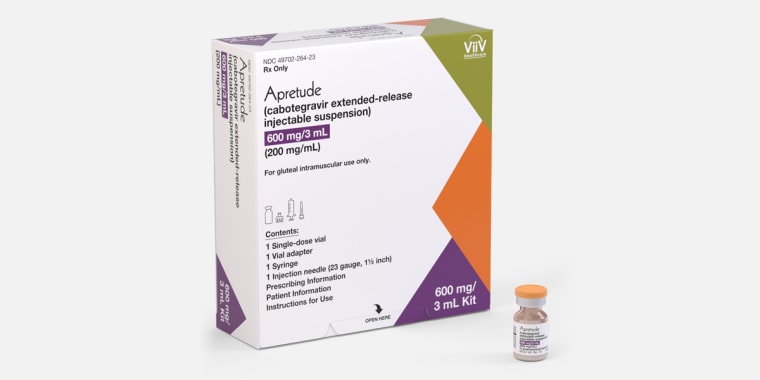
Approved in December 2021, Apretude requires receiving an injection by a health care worker every two months. Compared with providing trans women and men who have sex with men Truvada as PrEP, giving them Apretude was associated with a 66% lower overall HIV diagnosis rate in a major clinical trial.
Apretude’s superior efficacy was driven by the fact that participants adhered better to the injection schedule than to the daily pill regimen.
Dr. Hyman Scott, an HIV prevention expert at the San Francisco Department of Public Health, reported at the Seattle conference that of the 844 Black American participants in the trial, those randomized to receive the injectable drug had a 72% lower HIV rate than those who got Truvada.
His analysis suggests that if 10,000 similar Black gay and bi men and trans women were followed for one year, approximately 50 would contract HIV if given Apretude, while 200 would test positive if provided Truvada.
Such sobering findings about Truvada’s shortcomings are in keeping with previous studies finding relatively low rates of adherence to the daily PrEP regimen among Black gay men. Such data suggests that even if HIV prevention advocates succeeded in vastly increasing oral PrEP access in this population, it might have only limited impact among them.
Referring to Apretude, Scott told NBC News, “Whether we can get this rolled out in communities is the real question.”

Cost is a major rub. Since 2021, Truvada has been available from multiple generic manufacturers and now often costs as little as $25 to $35 per month, although in some cases up to $600. ViiV lists Apretude at $1,878 per month, and few insurers are covering it.
The recent CDC PrEP-use study presented in Seattle found that only about 1 in 200 PrEP prescriptions were for Apretude in September.
“There are patients who are getting Apretude now, but it’s people who have health care access, who have health care literacy, who call their insurance companies and yell at the right people,” said Dr. Anu Hazra, a physician at the LGBTQ-focused Howard Brown Health in Chicago.
Since 2021, almost all insurers have been obliged under the Affordable Care Act to cover oral PrEP with no out-of-pocket costs for the medications or the quarterly clinic visits and lab tests required to maintain a prescription. This is because in 2019, an advisory body known as the U.S. Preventive Services Task Force gave PrEP an “A” rating for being a worthy preventive tool.
In December, the task force issued a draft decision granting Apretude its own “A” rating. If this rating is made official this year, insurers will be required to cover Apretude, and with no cost sharing — but not until January 2025.
Apretude updates
In addition to the associated burden of having to come in six times per year for injections, Apretude does have a notable shortcoming: Breakthrough HIV cases are apparently much more likely among those taking injectable versus oral PrEP.
Of the 25 people who contracted HIV in the 2,282-person Apretude arm of the injectable-versus-oral PrEP trial among gay and bi men and trans women, six did so after getting their injections on schedule, according to a presentation in Seattle by Dr. Susan Eshleman, a professor of pathology at Johns Hopkins Medicine.
Eshleman’s team has not yet calculated the per capita Apretude breakthrough infection rate, but when these researchers initially reported last year that the trial saw seven breakthrough infections (before revising this figure down to six), their calculations suggested that if 10,000 similar men and trans women were followed for one year, 15 would contract HIV despite receiving on-schedule Apretude injections.
At the same Seattle conference, Hazra reported the first breakthrough HIV case in an Apretude patient outside of a clinical trial. By comparison, nearly four years passed after Truvada’s approval as PrEP before a breakthrough infection was first documented in someone faithfully taking that drug.
To date, there have been a handful of other case-study reports of breakthrough HIV in people taking oral PrEP. However, there has only ever been one clear such case in the major clinical trials including Truvada or Descovy as prevention.
All this suggests that for those with a history of taking daily oral PrEP on schedule, switching to Apretude would actually increase their HIV risk; although the absolute risk of infection would remain low.
Optimism in the pipeline
HIV prevention experts report excitement about the PrEP pipeline and expectations that in the coming decade, more convenient and longer-acting forms will be approved.
“I’m wildly optimistic,” said Sharon Hillier, a prominent HIV prevention researcher at the University of Pittsburgh. “We just have to work through how to deliver these interventions and how to be less burdensome for health care systems.”
The Seattle conference heard promising early stage research findings regarding medication-infused suppositories that could be placed into the rectum or vagina up to 48 hours following sex and likely prevent HIV. And researchers are developing implants that could be placed under the skin and emit preventive medication for many months.
Gilead is also running major PrEP trials of the drug lenacapavir, which requires an injection only every six months. Dr. Jared Baeten, who leads Gilead’s HIV strategy, said the company hopes to provide initial study results by 2025.
But if Apretude’s pacing is any guide, it could be 2030 before lenacapavir is both approved and widely covered by insurers.
In the meantime, PrEP advocates continue to express dedication to work with the options currently on the table, albeit within a complex and fractured health care system that proves alienating to many of those most at risk of HIV.

Benjamin Ryan